This research is especially relevant in light of a related paper out this week in the journal ScienceExpress: a collaborative effort between researchers at SeattleBioMed and Scripps Research Institute.
It is widely accepted that a successful vaccine against HIV/AIDS would have to elicit antibodies to prevent infection from a wide spectrum of HIV strains. So far, no candidate vaccine for HIV has been able to produce such antibodies.
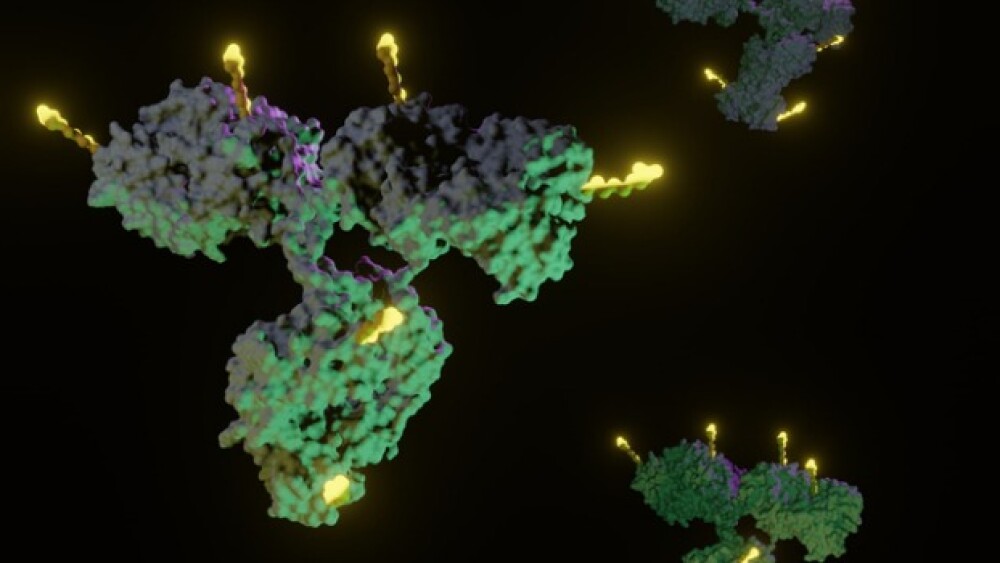
Leonidas Stamatatos, Andrew McGuire and their team of researchers at Seattle BioMed, in collaboration with colleagues at The Rockefeller University, the Scripps Research Institute and CalTech, wanted to understand why that was the case. A major goal of an HIV vaccine is to stimulate B cells to create antibodies that can effectively block HIV from entering a human host cell. The first generation of antibodies—called “germline antibodies”—are partially embedded in a B cell’s membrane. If a germline antibody binds to a protein (called an “envelope protein”) on the surface of HIV, even weakly, then the B cell is activated and begins producing antibodies not only on the surface of B cells, but also in the bloodstream. Activated B cells evolve to produce antibodies with even higher binding affinity to HIV, eventually resulting in a “mature” antibody. Some mature antibodies can bind to envelope proteins of many different HIV strains and prevent them from infecting cells. For this reason, these antibodies are called “broadly neutralizing antibodies”. These are the antibodies a vaccine needs to elicit.
A small number of people infected with HIV naturally produce broadly neutralizing antibodies. By sequencing the DNA of their mature antibodies, Stamatatos and McGuire were able to deduce what the originating germline antibodies likely looked like. They then tested how well the mature and germline antibodies bound to the envelope protein of different HIV strains from around the world. Some of these envelope proteins have been tested previously as vaccine candidates, but they did not elicit broadly neutralizing antibodies. While the mature antibodies were able to bind 80-90% of these diverse envelope proteins, the germline antibodies did not bind at all. This indicated that a problem with previously tested HIV vaccines is that they do not bind to germline antibodies on B cells that ultimately give rise to mature, broadly neutralizing antibodies. Without this first binding step, the immune response to HIV is stopped before it can even truly begin.
Next, they turned to the structure of the HIV envelope proteins to determine why they were able to bind to the mature antibodies but not the germline. They discovered that several sugar molecules, called glycans, which HIV adds to its envelope protein to evade the immune system, were blocking the germline antibody from binding to and activating B cells.
After engineering an HIV envelope protein that lacks specific glycans, McGuire and Stamatatos ran their binding tests again. This time, the germline antibodies were able to bind the modified HIV protein. They also verified that the modified HIV protein was capable of starting the process of antibody maturation in B cells, kicking off an immune response that could eventually result in broadly neutralizing antibodies.
“We have overcome the first obstacle to elicit one type of anti-HIV broadly neutralizing antibodies through vaccination,” explains McGuire. By administering the modified HIV protein as a vaccine, the immune system could become equipped to combat the real virus when it is encountered years down the line.
PRESS CONTACT
Hannah Krakauer
hannah.krakauer@seattlebiomed.org
206.256.7259
ABOUT SEATTLE BIOMEDICAL RESEARCH INSTITUTE Seattle BioMed is the largest independent, non-profit organization in the U.S. focused solely on infectious disease research. Our research is the foundation for new drugs, vaccines and diagnostics that benefit those who need our help most: the 14 million who will otherwise die each year from infectious diseases, including malaria, HIV/AIDS and tuberculosis. Founded in 1976, Seattle BioMed has more than 330 staff members. By partnering with key collaborators around the globe, we strive to make discoveries that will save lives sooner. For more information, visit www.seattlebiomed.org.